Dear Friends,
Thank you for taking time to go through this zone, which will help you to go a long way in planning for your Total Hip Replacement surgery. We are committed to deliver the finest and total care possible to ensure a complete recovery and early return to your day to day activities.
The information in this section is designed to help you understand more about total hip replacement. It is only intended to be a general guide and there will be variations from one case to another. It is therefore important that you discuss everything with an expert before your operation.
We are devoted to research and development and hence you are very valuable to us for providing such information throughout your life.
Please stay in touch even if you are far away from us.
 The hip joint is a ' ball and socket' joint. The hip joint allows movement to occur between the thigh bone (Femur), and the hip bone (Pelvis). The pelvis contains the 'socket' called the acetabulum. The ball shaped head of the femur fits into the acetabulum, forming a ball and socket joint which enables the leg to have a wide range of movements.
The hip joint is a ' ball and socket' joint. The hip joint allows movement to occur between the thigh bone (Femur), and the hip bone (Pelvis). The pelvis contains the 'socket' called the acetabulum. The ball shaped head of the femur fits into the acetabulum, forming a ball and socket joint which enables the leg to have a wide range of movements.
The outer surface of the femoral head and the inside surface of the acetabulum are covered with cartilage. The cartilage surface is a tough and very smooth material that allows the two surfaces to slide against one another during movement with ease.
Hip joint replacement surgery involves replacing the Head of the femur (ball) and the acetabulum (socket) with man made components, called prostheses. The hip prostheses are designed to simulate the human anatomy as closely as possible.
Depending on the damage to your hip, your surgeon may decide to give you a total hip replacement or a hip resurfacing procedure.
There are many different designs of hip prosthesis available and your surgeon will choose the one considered most suitable for you. However, the final decision may need to be made during the time of your operation.

X-Ray of a normal hip

X-Ray of arthritic hip before operation

X-Ray of replaced hip after
operation with bone graf
 Each hip prosthesis is made up of several parts:
Each hip prosthesis is made up of several parts:
The acetabular component or cup replaces the acetabulum. The acebular component can either be made of a metal alloy outer shell with a fitted plastics, metal or ceramic liner or it can be made of a one plastic component.
The femoral component replaces the femoral Head. The femoral component can be a single or two piece design. The single piece is made of metal alloy. While the two piece design consists of the femoral stem, made of metal alloy and the femoral head that attaches to the stem can be made of either ceramic or metal alloy. This is known as a modular prosthesis.
Envelopes of tough ligaments connect the pelvis and femur, covering the joint and stabilising it. The hip joints' movements are initiated and controlled by the thick muscles of the buttock at the back and thick muscles of the thigh at the front.
A healthy hip joint will allow the leg to move freely within it's range of motion, while supporting the upper body and absorbing the impact that results from activities such as walking and running.
 There are a number of conditions that can result in a patient having to undergo hip replacement surgery. Perhaps the most common condition is osteoarthritis that is commonly referred to as 'wear and tear arthritis'. Osteoarthritis can occur with no previous history of injury to the hip joint. The hip simply 'wears out'. There may be a genetic tendency in some people that increases their chances of developing osteoarthritis.
There are a number of conditions that can result in a patient having to undergo hip replacement surgery. Perhaps the most common condition is osteoarthritis that is commonly referred to as 'wear and tear arthritis'. Osteoarthritis can occur with no previous history of injury to the hip joint. The hip simply 'wears out'. There may be a genetic tendency in some people that increases their chances of developing osteoarthritis.
Avascular necrosis is another condition that could lead to hip replacement surgery. In this condition, the femoral head (ball) loses a portion of its blood supply and actually dies. This leads to collapse of the femoral head and degeneration of the hip joint. Avascular necrosis has been linked to alcoholism, fractures and dislocations of the hip, and long term steroid treatment for other diseases.
Abnormalities of hip joint function resulting from trauma to the hip, fracture of the hip, and some types of hip conditions that appear in childhood, such as congenital dysplasia of the hip (CDH) can lead to degeneration many years later. The mechanical abnormality leads to excessive wear and tear.
There are a number of ways in which the pain in your hip can be relieved. These can include changes in lifestyle or taking pain relieving medications. Another option is an operation to replace your hip joint. Replacing the hip joint is usually recommended when the pain becomes so constant that it is limiting your everyday activities and when you and your doctor agree that it is the best course of action.
The aim of hip replacement surgery is to:
→ Relieve your pain.
→ Correct any deformity.
→ Provide stability to your joint.
→ Restore loss of function in your hip.
→ Equalise leg length, if possible.
→ Improve your quality of life.
→ You must show all your Medicines to your doctor before operation. Some of the medicines may need to be discontinued temporarily before operation.
→ Stop smoking. If you have not already done so, it is suggested that you stop smoking at least four weeks before your surgery. This will help reduce the risk of complications during and after your surgery.
→ Make sure all infections are cleared up prior to the surgery. These include: tooth abscesses, bladder infections, infections such as leg ulcers, colds and the flu. This is because infections could spread through your body during the operation and infect your new replaced joint. Therefore you must notify your surgeon immediately if you are suspected or diagnosed with an infection, as they may have to reschedule your surgery.
You may also wish to consider how you will cope after the operation, for example, you may need help getting home, shopping, etc. Do discuss this with your doctor or a hospital staff member.
→ Commit to the success of your surgery: Working as a team, you, your physician, physiotherapist and your family must adopt a positive attitude toward the success of your surgery. Together, you will gain a clear understanding of the common goals and expectation of the procedure.
→ Remain as active as possible. Remaining active while waiting for your surgery is an important key to the success of your surgery. Studies have shown that the stronger and more flexible you are before your operation the quicker you will recover and more flexible you will be after the operation.
→ Gentle exercise such as walking, range of motion exercises and swimming can help you to stay strong and flexible. Seek your doctor's advice before beginning any exercise.
→ You need to improve your breathing by Incentive Spirometer.
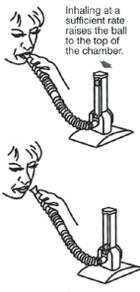
1. With the unit in an upright position, place your lips tightly around the mouthpiece and exhale normally.
2. To achieve a deep and sustained breath, inhale at a rate sufficient to raise the ball in the chamber.
3. Exhale. After performing the exercise, remove the mouthpiece from you lips.
4. Relax and breathe normally for a moment after each deep breath.
5. Repeat this exercise 10 times every hour
You should be admitted to hospital in good time before your operation to allow time for you to settle in. You will be examined by your anaesthetist, checking your heart and chest. This is an opportunity for you to ask any questions before your operation.
On the day of your operation, it is usual that your doctor will ask you not to drink or eat anything. The area around your hip may be shaved to reduce the risk of infection.
An hour or so before the operation you will be given tablets or an injection to relax you. This is known as a 'pre-med'. You will then be taken into the operating theatre where you will be given your anaesthetic and have your operation.
The operation usually takes 1-2 hours to complete.
Immediately after your operation you will be moved to the recovery room for close monitoring. You will have one or two drips in your arm to put fluid back into your body. When you wake up from surgery, your leg may be swollen and bruised and the muscles may be stiff and sore. Your new joint should not cause you any discomfort, but you may experience some pain from the surgical procedure itself. You will be given pain medications to take regularly whilst you are recovering.
When you are fully conscious, breathing well and your blood pressure and pulse are stable, you will be taken back to ward. You probably won't feel much like eating at first, but it is important that you drink. The scar on the side of the hip should eventually fade to a thin white line. During the next few days the drips will be removed. Your physiotherapist will visit you the day after your operation to commence you on your exercise programme and help you get back on your feet walking again. You may feel unstable and in pain at first, but you will be given a frame to help you walk with, then crutches or sticks, which you may need for four to six weeks after, depending on your surgeon's instructions.
Once you, your surgeon and physiotherapist are happy with your condition and mobility you will be discharged from hospital. The usual hospital stay for hip joint replacement is usually four to seven days.
Upon returning home you will need help for the first few weeks and should make arrangements for someone to shop for you and help you around the house. You will need to continue taking your regular medications and continue exercising as directed by your physiotherapist and surgeon.
Remaining active and practicing the prescribed exercises are the quickest ways to full recovery.
You have every reason to expect to regain full use of your leg. However this will take time. You should be able to return to normal activities again within a few months of the operation. These may include driving, gardening and playing golf, but check with your doctor first. There will be a continual improvement throughout the first 12 months. Once the operation has fully healed, many people can't tell they have an artificial joint !!
Every effort is made to minimise any risk or complications from occuring. However, like any other surgery they do occur. Listed below are common signs and symptoms that may indicate a complication with your new joint. Please contact your doctor should you feel that you may have problem or are experiencing any of these signs and symptoms:
→ Fever of 101 degrees Fahrenheit or 38.3 degrees Celsius.
→ Unusual redness, heat or oozing at the wound site.
→ Trouble breathing or shortness of breath.
→ Increase in pain that is not relieved by medication.
→ Increase in pain or swelling in the calf.
→ Increase in swelling of the leg that is not relieved by elevation.
The Food Guide Pyramid (illustrated here) is an outline of what to eat each day. It helps you choose a healthful diet that is right for you. The Food Guide Pyramid is based on the recommended dietary guidelines for Americans. Use the Food Guide Pyramid to make your daily food choices. The Pyramid encourages you to eat a variety of foods, which will provide the nutrients you need and the right amount of calories to maintain a healthful weight.

The Food Guide Pyramid emphasizes foods from the five food groups shown in the lower three levels of the Pyramid. Each of these food groups provides some, but not all of the nutrients you need. No one food group is more important than another; for good health you need them all.
→ Do I need a joint replacement surgery?
If you have arthritis, which is quite bothering you in your day to day activities even during sleep, probably you will benefit from the operation. But your doctor has to examine you and see your X-rays to finally decide about the surgery.
→ Do I need to prepare myself before surgery?
You need to be investigated in order to be fit for anaesthesia. Moreover, you should practice certain exercises like deep breathing etc. to avoid complications after surgery. Our team of experts will assist you in pre and post operative precautions and guidelines.
→ What exercises I need to do after surgery?
We shall make you walk with support about 2-3days after your surgery. Moreover, you will start to bend your new joint and do the movements during the same time. We shall take care of your pain by different medications and you will be able to do it with the help of our expert team of physiotherapists and occupational therapists.
→ What are the disadvantages of this operation?
There is less than 1% chance of infection in the world's best centres. We match the international standards by having strict operation theatre protocol, antibiotics, infection control team and discipline in the ward itself. Other complications are minor and it is possible to avoid if you strictly follow the advice of your doctor and therapists.
→ How long an artificial joint last?
We give an average life span of about 10-15 years. But the longest surviving artificial joint is 40 years in the world. It also depends on how you take care of your new joint.
→ Will it affect my day to day life?
The surgery will lead to better quality of life and you can do your day to day activities normally.
For any other queries, you can send e-mail. In case of emergency, please don't hesitate to contact on cell phone.

