The knee joint is among the strongest, largest and most complex joints of the body. Whenever you walk, sit, squat, turn around, drive or perform many other seemingly simple movements, you are depending on the knee for support and mobility. When your knee is healthy, you may take it for granted, not giving a thought about the job it does for you. But once it starts to become painful, stiff, and you are forced to restrict certain activities, you may come to realize how much freedom of movement means to you.
Fortunately, today's advanced medical technology makes it possible to replace the knee joint with an artificial one that reduces pain, allows you to strengthen your legs, and improves your quality of life.
Knee replacement is a procedure commonly performed throughout the world, and one that offers an outstanding rate of success.
In this section, we will discuss how your knee works, how arthritis causes your pain and the knee replacement surgery you will have. We will also help you make preparations for the upcoming surgery and outline what you can expect every step of the way.
How Your Knee Joint Functions?
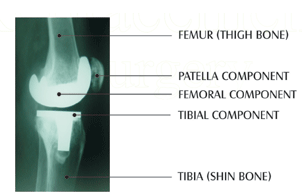
The healthy knee. The healthy knee joint is a remarkable mechanism. It is formed by the bottom end of the femur (thigh bone), the top end of the tibia (shin bone) and the patella (knee cap). A healthy knee joint has cartilage between the bones that acts as padding. This padding helps assure a gliding movement of the knee that is both effortless and smooth. The healthy knee joint also has a joint capsule which houses the synovial membrane. This membrane produces lubricating fluid which contributes to the smooth movement of the knee.
The human knee is designed to withstand a lifetime of stressful activity. However, sometimes arthritis intrudes, interfering with the knee's ability to cushion the body from stress, and eventually causing the pain that dramatically erodes your quality of life.
Arthritis is not a symptom of "just getting old". It is a degenerative or inflammatory disease of the joints that is not necessarily part of the normal aging process. Indeed, some patients with arthritis present symptoms in their 20s and 30s. Although there are several types of arthritis, one of the most common is called osteoarthritis. It affects millions of people in the world today.
Arthritis causes permanent deterioration of the cartilage layers that shield the joint from impact. Because cartilage cannot repair or replenish itself, it begins to crack, wear away and eventually disappear. The cushion your knee requires to absorb stress is gone, resulting in bone-on-bone contact. The bones in advanced cases may be so Rough and pitted from grinding against each other that they form bone spurs, which often cause stiffness.
In the first stage of osteoarthritis, your knee may feel stiff and swollen. Later, you may feel pain and may notice that one leg seems shorter or more crooked than the other. Eventually, your mobility may become limited and you may need to alter your lifestyle to accommodate your sore, arthritic knee. If you are overweight or have a malalignment, the extra stress on your knee can accelerate the damage.
Regardless of your type of arthritis, you may have already had to curb or quit the activities you enjoy. This is partly why arthritis can make people "feel" old, even though they are still in the prime of life. But there is hope-you have options.
Total knee replacement surgery is an elective procedure. Along with your doctor, you will decide when the time is right for this surgery. Your doctor has more than likely treated your condition with plain medications, anti-inflammatory drugs or perhaps even minor surgery. But now the pain has become severe. Even staying off your feet doesn't help. You cannot sleep at night because of the discomfort. You are probably the best judge of when you will finally need total knee replacement surgery. When the pain becomes so chronic that even medication does not seem to help, you are probably ready to consider surgery.
Take the four essential steps that will help you get into shape before knee replacement surgery.
→ Commit to the success of your surgery: Working as a team, you, your physician and your family must adopt a positive attitude toward the success of your surgery. Together, you will gain a clear understanding of the common goals and expectations of the procedure.
→ Lose excess weight: Because excess weight causes strain to be placed on already-damaged joints, losing weight is one of the best ways to improve the condition of your knee and optimize surgical results. Remember to seek your doctor's advice before beginning your weight loss program.
→ Start a physician- approved, low-impact exercise plan. After a comprehensive assessment of your condition, your physician or physical therapist may recommend a low-impact exercise plan that will strengthen your knee without creating further damage. Do not attempt an exercise program without consulting your physician!
→ Stop smoking. If you have not already done so, it is suggested that you stop smoking. This will be good for you during and after surgery.
Surgery and manufacturers have made remarkable advances in joint replacement technology over the last few years. The materials are long-lasting and durable. The surgical aspects have been fine-tuned, the chances for a successful outcome are excellent.
In total knee replacement (also known as total knee arthroplasty, or TKA), the joint's bone-end surfaces are resurfaced with man-made materials. In total knee arthoplasty, the implant (prosthesis) design may vary according to your needs, but the most common implant consists of three omponent parts. The patella, or knee cap, is made of high-density polyethylene, which offers tremendous strength and durability. The femoral section, or thigh bone, is metal, while the tibia, or shin bone, is made of high-density polyethylene and may be supported by a metal tray.
Once your new joint has completely healed, you will reap the benefits of the surgery. These include:
→ Reduced joint pain (may be no pain!)
→ Increased movement and mobility for e.g. Walking, stair climbing, etc.
→ Stable Joint.
→ Straight Joint (Correction of deformity)
→ Increased leg strength (if you exercise)
→ Improved quality of life-ability to return to normal activities and pastimes.
Most likely, running, jumping, or other high impact activities will be discouraged.
As with any major surgery, there are potential risks involved. It is important that you are informed of these risks before the surgery takes place,
→ Infection: Because a bacterial infection from any part of your body could infect your new joint, you will be asked to complete all investigations before surgery.
→ Consult your physician before scheduling any pre or post operative dental work.
→ Blood clots: You could develop blood clots. Many TKA surgeons perscribe anticoagulation medications after surgery . You may also need to wear elastic stockings for several weeks to minimize the risk of blood clots forming and to prevent emboli.
→ Restore loss of function in your hip.
→ Pneumonia: Pneumonia can sometimes develop in patients who are lying in bed right after surgery. Getting out of bed soon after surgery is encouraged.
Medical Evaluations: Before surgery, your doctors need to understand your overall health status. You will be evaluated in several ways,
→ Complete medical evaluation: Your doctor will take your health history, an inventory of medications you now take, and will do a total physical examination X-ray images will be taken of your knee that help the surgeon plan your surgery. Some patients will also need chest X-rays, ECGs and other tests to ensure they are strong enough for surgery and recovery.
→ Preliminary lab work: As part of your pre-admission process, you will need to undergo routine lab work. Your physician's nurse can explain what each test is and why you need it.
→ A note about medications: It is very important to tell your doctor about every single medication you are taking, even aspirin or ibuprofen. Some medications are not compatible with anaesthetic, and others could increase bleeding or cause other problems. Your physician will determine which medications you can continue up until your surgery, and which ones you must discontinue.
When packing your hospital bag, bring your list of medications and the telephone numbers of your relatives or designated "help" person. Bring walking shoes, loose, comfortable clothes, underwear, books, personal care items and cash for sundries. Please don't bring jewelry, large amounts of cash, credit cards or other valuable items to the hospital with you.
What To Expect Right After Surgery? In the recovery room, you will recover from surgery until you are awake and alert. You could experience chills or nausea-these are normal side effects of anesthesia. You may notice:
→ Drainage tubes and catheters: A drainage tube and catheter may be in place.
→ Pain medications: To manage the pain you may feel right after surgery, you will be given medication.
→ Elastic stockings: You may be fitted with elastic surgical stockings that help prevent blood clots and improve circulation. You may wear these stockings every day for six to eight weeks following surgery.
→ CPM machine: Your operated leg may be connected to a CPM (continuos passive motion) machine, which slowly bends it up and down to improve range of motion.
You are returned to your regular hospital room once you are completely awake. Your family members may then visit you in your room. Deep breathing: It is important to exercise your lungs to make sure your air passages are clear. You can do it with incentive spirometer.
Two Days After Surgery
IV tubes and lines are usually removed within the first few days following surgery. If a drain was placed in your knee, then it will probably be removed a day or two after surgery. The start of physical therapy. Physical therapy usually begins for most patients within the first few days following surgery. The therapist focuses on helping to increase the knee's range of motion with bending exercises. You will also be building strength in the knee and muscles of the leg. Often the CPM machine is continued at a higher degree of bend.
Three To Four Days After Surgery
Your physical therapy will continue, except you will practice becoming more independent in your exercises, transfers from bed to chair, stair climbing and other activities your therapist has designed for you. Your dressing will be changed, as well as your blood tested for coagulation. Before you are discharged from the hospital, your physician and physical therapist will review instructions for your continuing care and exercises at home. You will be given prescriptions for medication you need.
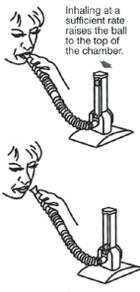
1. With the unit in an upright position, place your lips tightly around the mouthpiece and exhale normally.
2. To achieve a deep and sustained breath, inhale at a rate sufficient to raise the ball in the chamber.
3. Exhale. After performing the exercise, remove the mouthpiece from you lips.
4. Relax and breathe normally for a moment after each deep breath.
5. Repeat this exercise 10 times every hour
Your knee replacement should give you years of service. You can protect it by taking a few simple steps:
→ Watch for and prevent: Because your new knee is sensitive to infections, you must be diligent about preventing them. You may need to take antibiotics before seeing the dentist. If you suspect a bacterial infection of any kind, notify your physician right away.
→ Follow-up care: When you leave the hospital, you will be given schedule of follow-up visits. These visits will ensure the long-term success of your operation. Your physician may want to check you several times during the first year and annually thereafter. Often, follow-up X-rays will confirm proper placement and alignment of the implant.
→ Weight control: Keeping your weight under control will reduce the amount of pressure and stress on your new knee. Avoid high-impact sports and participate regularly in low-impact activities such as walking, swimming, golfing or cycling. These are excellent ways to strengthen your new knee and get the exercise you need to stay fit.
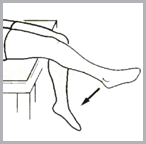
→ Sit on the edge of a table or chair.
→ Try to bend your operated knee as much as you can, assisting with the opposite leg.
→ Hold for 10 seconds.
→ Do 15 repetitions, 3 times per day.
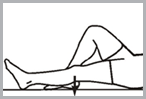
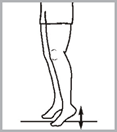
→ Sit or lie on your back with your leg straight.
→ Press the back of your knee downward. This will tighten the muscle on top of your thigh and move your kneecap.
→ In a sitting position, press your knee down using both hands to apply additional pressure.
→ Hold for 10 seconds.
→ Do 15 repetitions, 3 times per day.
→ Place your foot on a low stool.
→ Lean your weight forward to bend the knee so that you can feel a stretch.
→ Hold for 10 seconds.
→ Do 15 repetitions, 3 times per day.
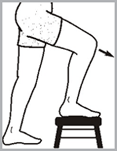
→ Stand up, holding on to something sturdy.
→ Raise yourself up onto the balls of your feet.
→ Hold for 10 seconds.
→ Do 15 repetitions, 3 times per day.
Every effort is made to minimise any risk or complications from occuring. However, like any other surgery they do occur. Listed below are common signs and symptoms that may indicate a complication with your new joint. Please contact your doctor should you feel that you may have problem or are experiencing any of these signs and symptoms:
→ Fever of 101 degrees Fahrenheit or 38.3 degrees Celsius.
→ Unusual redness, heat or oozing at the wound site.
→ Trouble breathing or shortness of breath.
→ Increase in pain that is not relieved by medication.
→ Increase in pain or swelling in the calf.
→ Increase in swelling of the leg that is not relieved by elevation.
The Food Guide Pyramid (illustrated here) is an outline of what to eat each day. It helps you choose a healthful diet that is right for you. The Food Guide Pyramid is based on the recommended dietary guidelines for Americans. Use the Food Guide Pyramid to make your daily food choices. The Pyramid encourages you to eat a variety of foods, which will provide the nutrients you need and the right amount of calories to maintain a healthful weight.

The Food Guide Pyramid emphasizes foods from the five food groups shown in the lower three levels of the Pyramid. Each of these food groups provides some, but not all of the nutrients you need. No one food group is more important than another; for good health you need them all.
→ Do I need a joint replacement surgery?
If you have arthritis, which is quite bothering you in your day to day activities even during sleep, probably you will benefit from the operation. But your doctor has to examine you and see your X-rays to finally decide about the surgery.
→ Do I need to prepare myself before surgery?
You need to be investigated in order to be fit for anaesthesia. Moreover, you should practice certain exercises like deep breathing etc. to avoid complications after surgery. Our team of experts will assist you in pre and post operative precautions and guidelines.
→ What exercises I need to do after surgery?
We shall make you walk with support about 2-3days after your surgery. Moreover, you will start to bend your new joint and do the movements during the same time. We shall take care of your pain by different medications and you will be able to do it with the help of our expert team of physiotherapists and occupational therapists.
→ What are the disadvantages of this operation?
There is less than 1% chance of infection in the world's best centres. We match the international standards by having strict operation theatre protocol, antibiotics, infection control team and discipline in the ward itself. Other complications are minor and it is possible to avoid if you strictly follow the advice of your doctor and therapists.
→ How long an artificial joint last?
We give an average life span of about 10-15 years. But the longest surviving artificial joint is 40 years in the world. It also depends on how you take care of your new joint.
→ Will it affect my day to day life?
The surgery will lead to better quality of life and you can do your day to day activities normally.
For any other queries, you can send e-mail. In case of emergency, please don't hesitate to contact on cell phone.

